Mechanism of Action
1. Osteoclast
- Attracted to areas of ‘micro-damage’ where its ruffled border attaches to create a sealed cavity.
· Via an energy dependant process carbonic acid and matrix degrading enzymes are secreted in to this sealed cavity causing bone resorption.
- Following bone resorption by osteoclast, osteoblast lay down osteoid that subsequently forms new bone.
· Osteoclast are stimulated by RANKL which is produced both by osteoblast and osteocytes.
2. Osteoblast
- Osteoblast activity is influenced by osteocytes.
3. Osteocytes
· The most abundant cell type in bone. They form an interconnected network in mineralised bone.
· They respond to mechanical changes applied to bone and are often referred to as the ‘mechanostat’.
o Respond to mechanical change on bone.
- Secretes
· Sclerostin that has an inhibitory effect on bone formation by blocking osteoblast function. When bone is loaded, there is a decrease in sclerostin secretion and this results in increased bone formation by osteoblast via the Wnt pathway.
· RANKL secretion, in contrast, is increased when bone is unloaded. This stimulates osteoclastic mediated bone resorption.
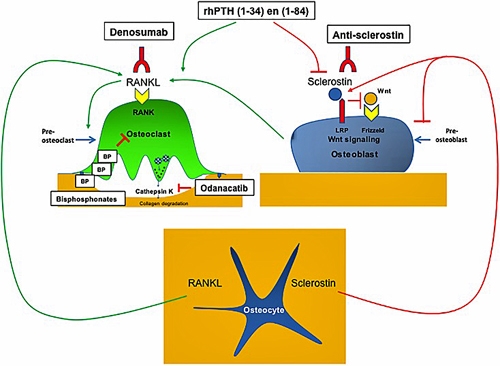
Figure 2. Diagram demonstrating the effect of antiresorptive and osteoanabolic drugs on bone.