- Human (Figure 12) or animal
- Multiple infective species
- Broad spectrum antibiotics. Often wound washout is needed for hand bites (“fight bites”)
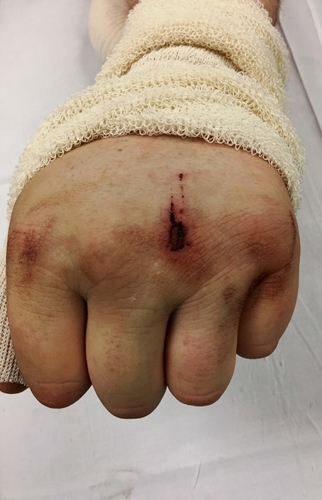
Figure 12. Clenched-fist injury. Also known as a fight-bite injury, this serious injury typically is characterized by a 3- to 5-mm laceration on the dorsum of the hand or overlying the metacarpophalangeal joint.