.jpg)
.jpg)
Figure 13 (a) and (b). Back & side View of AFO with cut out heel
Indications: Similar to AFO’s for Foot Drop, tendon Reconstruction/ Repair but allows eel to be cleared to avoid get pressure sores at heel. Not rigid enough so not suitable for deformity correction and severe OA / degeneration of Ankle.
.jpg)
.jpg)
Figure 14 (a) and (b). Example of a Dynamic Short AFO which makes rocking motion possible because of the gel insert (blue coloured) which attaches on the outside of the thermoplastic splint.
Benefits: balance enhancement, fits a variety of footwear
Features: light weight, cleanable
Considerations: indicated for mild foot drop
.jpg)
.jpg)
Figure 15 (a) and (b). Carbon Fiber AFO with rear entry (note padding at front) with foot elevated off the ground to allow to provide a rocking motion.
Bracing for Degenerative Ankle Joint /OA of Ankle:
Order of Bracing : rigid and sturdy to lightweight with less control. Rigid and sturdy as a principle is good for severe disease while less sturdy for early disease but not vice versa.
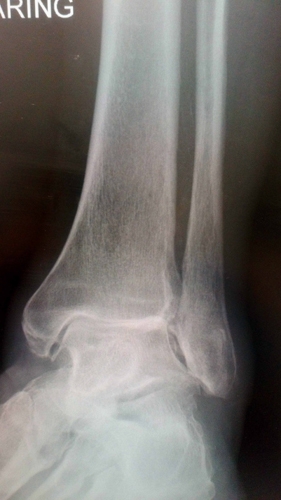
Figure 16. OA ankle
1st Line: AFO with Laces: e.g ARIZONA AFO
Benefits: excellent control, comfort
Features: durability
Considerations: may require an extra depth/width shoe

Figure 17. The Arizona AFO™ stabilizes the ankle, talocalcaneal, midtarsal and subtalar joints
2nd Line: Slim /Light Weight Brace: e.g AZ Breeze
Benefits: good control, slim design for easier shoe fit
Features: light weight, washable
Considerations: less durable than leather, unable to heat to modify pressure spots

3rd Line: Articluated allowing some movement at Ankle Joint
Benefits: enhanced mobility, excellent control
Features: lightweight, fits a variety of footwear
Considerations: not indicated for severe DJD or when support for the medial longitudinal arch is required

Figure 19. Arizona Articulated AFO. The Articulated Arizona AFO is designed to stabilize the subtalar, talocalcaneal, and midtarsal joints while still allowing motion at the ankle. It is available with a variety of ankle joints and stops.
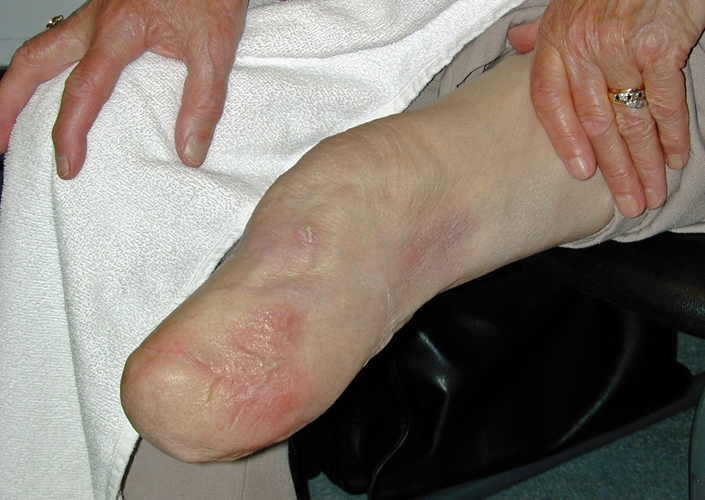
Figure 20. The successful fitting of Transtibial prosthesis is dependent on the fit of the hard socket. . Casting is used to help create a well fitting socket when an Iceross liner is being used. Inspect residue limb.Knowledge of anatomical landmarks,scarring and sensitive areas will aid in socket fitting.
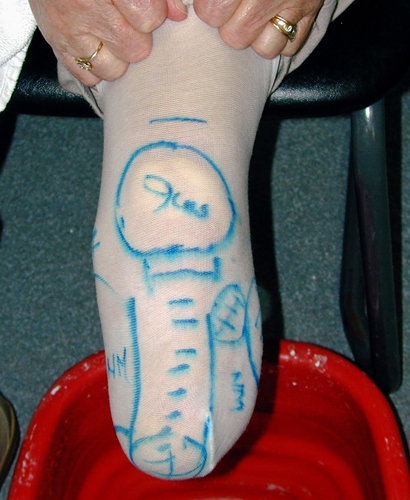
Figure 21. Identify and mark the following:
- Patella
- Fibulla head
- Crest of tibia
- Other bony areas that may contact socket wall
- Sensitive areas
- Neuroma
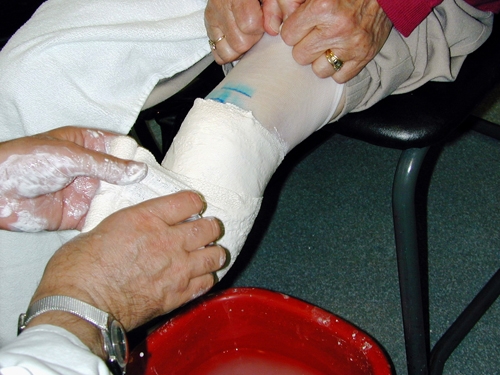
Figure 22. The knee should be extended but relaxed.Apply Plaster of Paris to cover distal stump
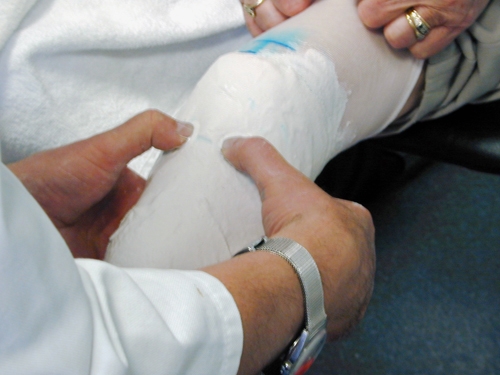
Figure 23. Mould plaster from anterior to posterior defining the bony prominences and capturing residue limb shape

Figure 24. Modification of cast.Strip cast and ensure all marks are transferred to positive.

Figure 25. Workshop

Figure 26. Hip disarticulation prothesis.Amputations through the hip are commonly referred to as hip disarticulations
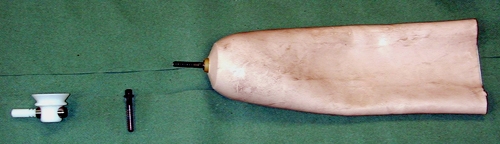
Figure 27. Transfemoral silicone locking prosthetic liner(Iceross) and pin
.jpg)
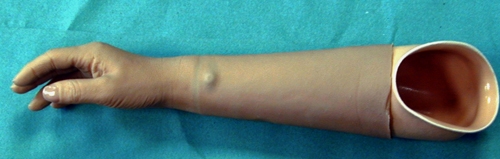
Figure 28 (a) and (b). Above elbow exoskeleton prosthesis

Figure 29. Above knee prosthesis.Transfemoral amputations are performed below the hip and above the knee.

Figure 30. Below knee prosthesis.transtibial amputations are performed below the knee and above the ankle

Figure 31. Above knee exoskeleton prosthesis

Figure 32. Various upper limb prostheses