Case based Discussion Renal Cell Mets
An active 62 year man presents to his GP with 8 weeks of pain in the left knee. He has tried physiotherapy but this has not helped. The GP refers him to a knee surgeon who performs the following X-ray
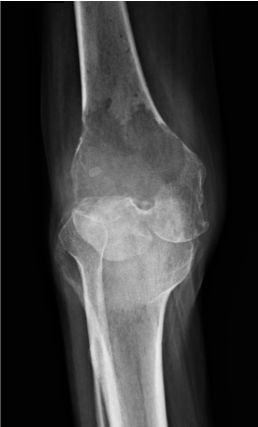
Anteroposterior(AP) radiograph knee
Examiner :The knee surgeon decides this warrants further investigation. Among other tests she orders a set of bloods. Which bloods would be appropriate?
Candidate:Standard FBC, U&E, coagulation screen. Bone profile to look especially for hypercalcaemia. Given the patient’s age, metastatic disease is high on the list of differentials. Tumour markers include CEA (bowel), Ca19-9 (pancreas), electrophoresis (myeloma), PSA (prostate), Ca125 (ovarian - if this was a female patient)
Examiner:What is Mirel’s score? How does it influence management?
Candidate:Mirel’s score is a set of criteria used to predict whether a bone containing a tumour will break. It assigns scores based on the lesion’s site, pain, size, and whether it is blastic or lytic. An increased score corresponds to an increased fracture risk.
Examiner:A CTCAP shows a mass in the left kidney, and renal cell carcinoma is diagnosed. Due to Mirel’s score, you feel that operative intervention is appropriate. Is there any procedure you would consider arranging prior to surgery? Which other diagnoses would you consider this for?
Candidate:Embolisation prior to surgery can reduce bleeding in highly vascular tumours such as renal, thyroid, and phaechromacytoma.